Abstract
Introduction: Procedural competence is central to medical training, and managing complications is essential for patient safety and physician wellness. We surveyed residents and fellows across specialties to evaluate formal and informal complication-management training and assess whether formal training improves comfort and preparedness.
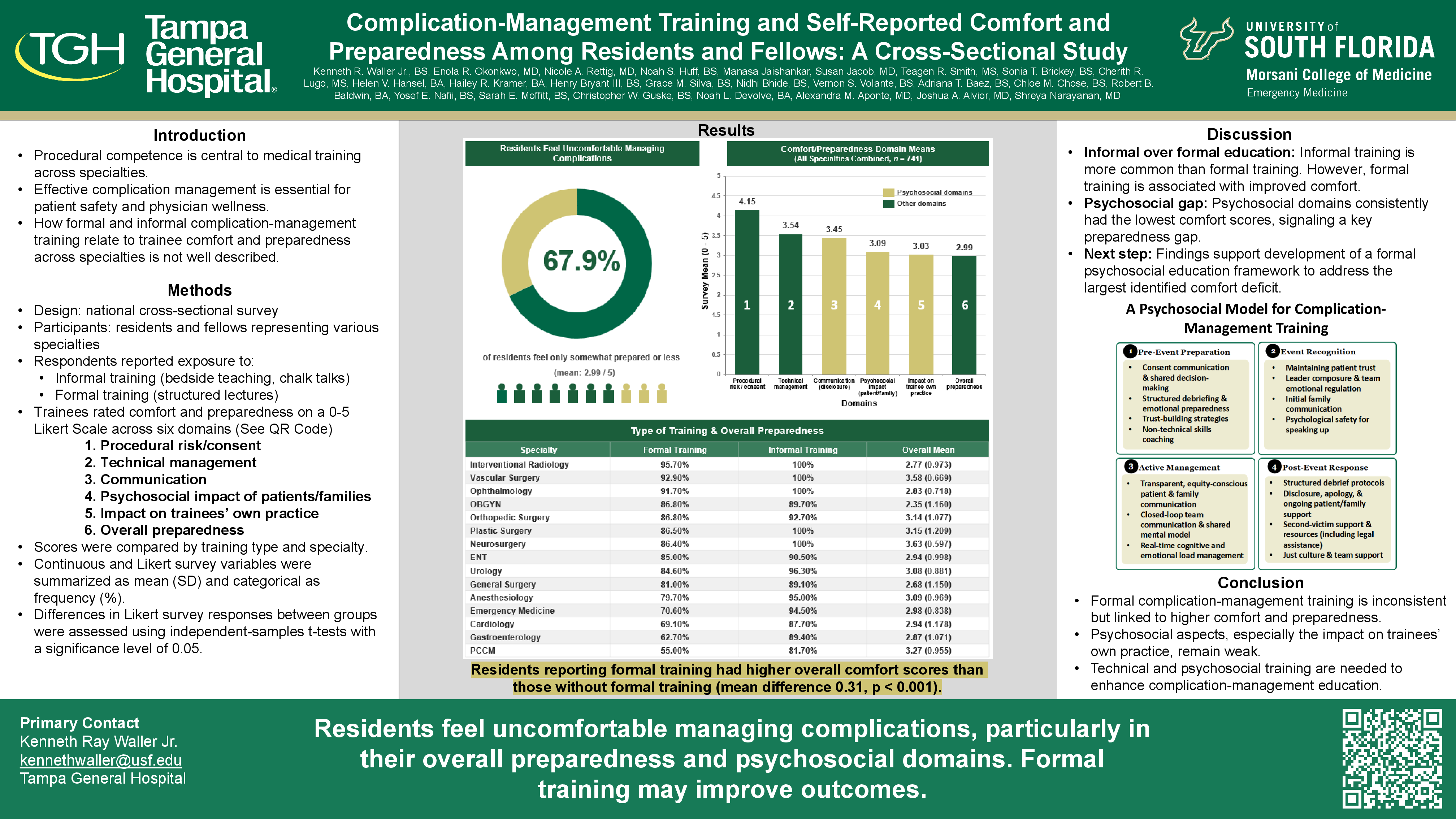
Methods: We conducted a national cross-sectional survey, to which 741 residents and fellows across various specialties responded. Participants reported exposure to informal (bedside teaching, chalk talks) and formal (structured lectures) complication-management training and rated their comfort and preparedness on a 0-5 Likert scale in six domains: procedural risks/consent, technical management, communication, psychosocial impact on patients/families, impact on their own practice, and overall preparedness. Scores were compared by training type and specialty.
Results to Date: Formal training varied by specialty, ranging from 55.00% reported in pulmonary critical care fellowship to approximately 95.70% reported in interventional radiology. Overall, 82.5% of trainees reported informal training. Comfort was highest for procedural risks/consent (4.15 ± 0.82) and technical management (3.54 ± 0.91), and lowest for psychosocial domains, particularly those related to the personal impact of complications on trainees (3.03 ± 1.03). Across all specialties, trainees with formal training reported higher overall preparedness than those without formal training (overall 3.12 ± 0.99 vs 2.59 ± 1.12; p<0.001).
Conclusion: Formal complication-management training is inconsistent but linked to higher comfort and preparedness. Psychosocial aspects, especially the impact on trainees’ own practice, remain weak. Structured, specialty-sensitive curricula integrating technical and psychosocial training are needed to enhance complication-management education.