Abstract
Purpose: Retroperitoneal sarcomas (RPS) present a unique challenge due to their large size and location in relation to many sensitive organs. Therefore, strategies to improve treatment plans and delivery are desirable. A treatment planning study was performed to evaluate the performance of volumetric modulated arc radiotherapy (VMAT) against sliding window IMRT on RPS patients.
Methods and materials: CT datasets of ten RPS patients treated with neo-adjuvant radiotherapy in 2012-2013 were obtained. New IMRT and VMAT plans were generated and calculated using the AAA algorithm in Varian Eclipse v. 11.0.31. Plans were optimized to deliver ≥ 95% dose to the PTV, while respecting QUANTEC based organs at risk (OAR) dose constraints for kidney, liver, spinal cord, and bowel space. Plans were evaluated for homogeneity as estimated by the van’t Riet conformity index (CI) and on pre-defined parameters obtained from dose-volume histograms. Mean dose to the unspecified tissue was recorded to estimate the integral dose. Mean doses at 1 cm, 2 cm and 5 cm from PTV were recorded to estimate dose fall-off. Monitor unit (MU) values were recorded and treatment delivery times were measured to estimate the efficiency. A two-tail Student’s paired t-test was performed to evaluate the difference between plans.
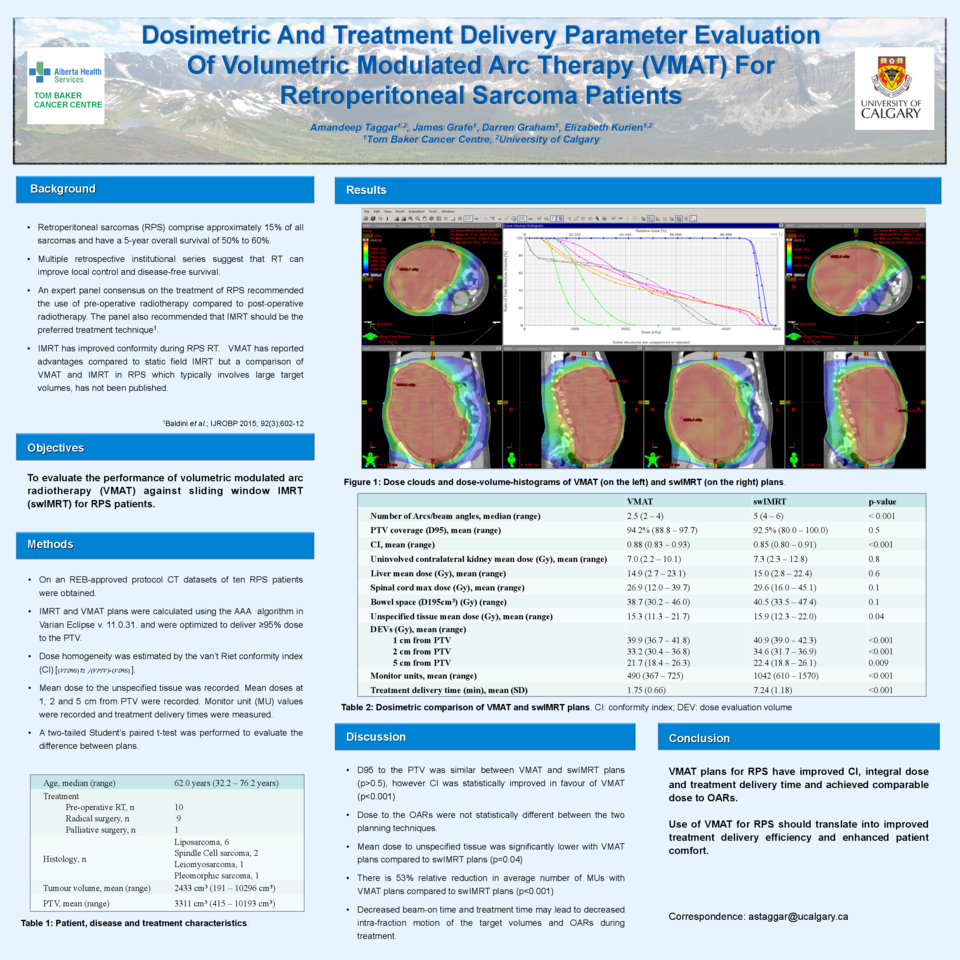
Results: Mean tumour volume was 2875 cm3, (standard deviation SD=3471) and mean PTV was 3311 cm3 (SD=3287). Both VMAT and IMRT generated plans with equivalent coverage of PTV (P=0.5). However, VMAT plans had better CI, 0.88 (SD=0.03) versus 0.85 (SD=0.03) (P<0.0001). Dose to the OARs was not significantly different for VMAT plans compared to IMRT plans: kidney, Dmean= 699 versus 728 cGy (P=0.8); liver, Dmean= 1484 versus 1500 cGy (P=0.6); spinal cord, Dmax= 2694 versus 2962 cGy (P=0.14); bowel space, V195= 3872 versus 4046 cGy (P=0.11); and unspecified tissue, 1530 versus 1590 cGy (P=0.04). Mean doses (SD) at 1 cm, 2 cm and 5 cm from PTV were 3990 cGy (164), 3323 cGy (170) and 2169 cGy (271) for VMAT plans versus 4094 cGy (130), 3426 cGy (133) and 2236 cGy (239) for IMRT plans (P<0.01). Average MUs for VMAT plans were significantly lower than IMRT plans (490 versus 1042 MU, P<0.0001). Similarly, average beam-on time to deliver VMAT plan was 1.75 minutes (SD=0.66), which is significantly lower compared to IMRT plans that required on average 7.24 minutes (SD=1.18) of beam-on time (P=0.001).
Conclusion: VMAT plans for RPS have improved CI, comparable dose to OARs, less integral dose and are deliverable in significantly less time. This should translate into improved treatment delivery efficiency and enhanced patient comfort.