Abstract
Background: Lower socioeconomic status (SES) and skin of color (SOC) patients experience poorer outcomes in melanoma and non-melanoma skin cancers, as well as disparities in sun protection education, knowledge, and preventive behaviors. Compared with White patients, Black patients with cutaneous squamous cell carcinoma have demonstrated longer treatment delays and larger Mohs surgery defects. Melanoma survival rates are lower in SOC patients despite higher incidence among non-Hispanic White populations. Lower SES is also associated with increased mortality and more advanced disease at presentation.
Objective: To explore factors contributing to healthcare disparities in skin cancer outcomes and inequities in sun protection education, prevention, and knowledge among lower SES and SOC patients.
Methods: A narrative literature review was conducted using combinations of relevant keywords in Google Scholar and PubMed. Articles were uploaded to ResearchRabbit for organization and review. Studies were screened by abstract relevance, and 20 articles were selected for in-depth review.
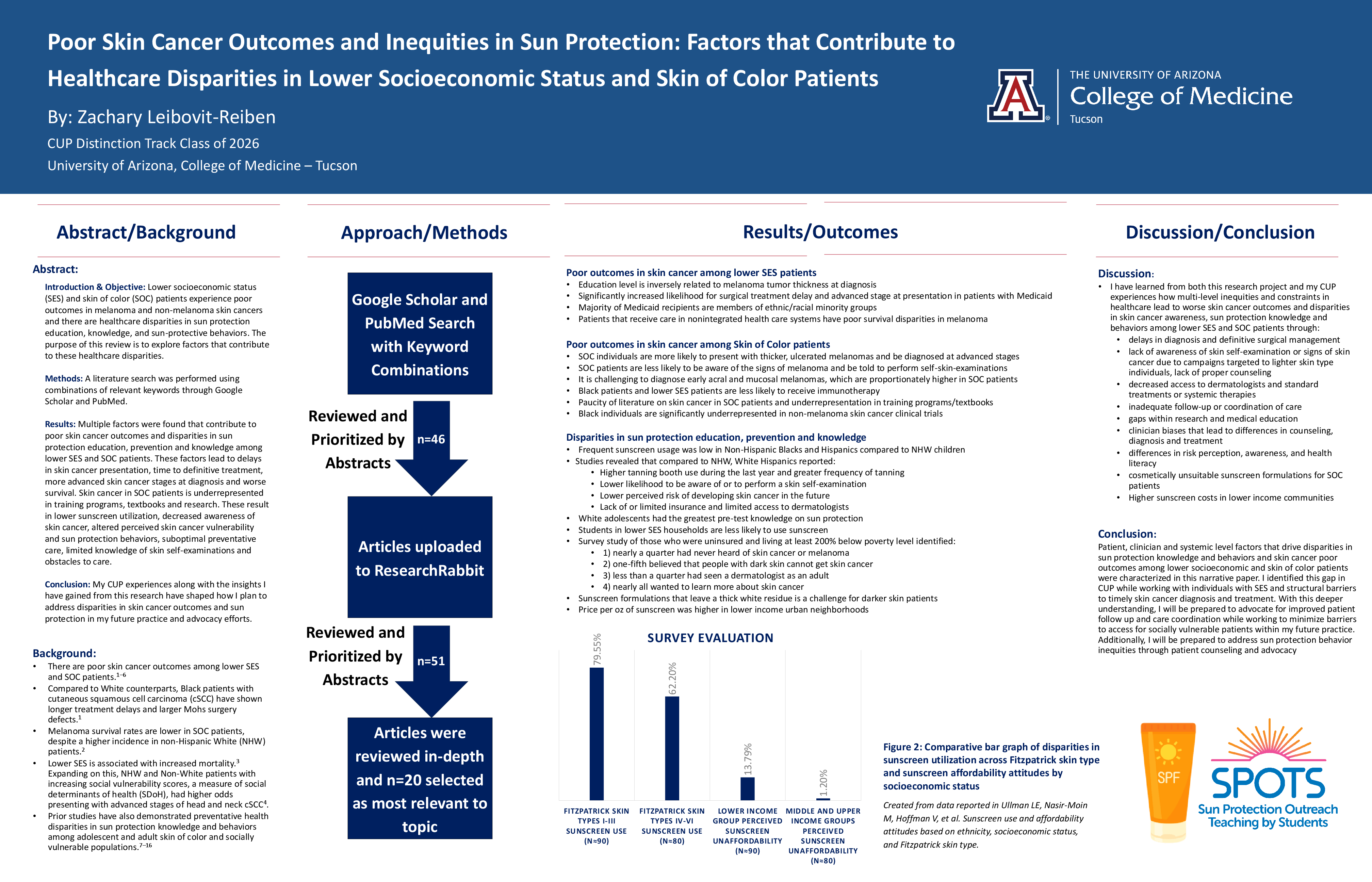
Results: Multiple patient-, clinician-, and system-level factors were identified as contributors to poor skin cancer outcomes in lower SES and SOC populations. These included delayed presentation, longer time to definitive treatment, advanced stage at diagnosis, and worse survival. SOC patients were more likely to present with thicker, ulcerated melanomas and were less likely to receive counseling on self-skin examinations. Skin cancer in SOC patients remains underrepresented in medical training, textbooks, and research, contributing to lower awareness and diagnostic challenges. Preventive disparities included lower sunscreen use among SOC and lower-income groups, higher perceived sunscreen unaffordability, limited access to dermatologists, lower perceived skin cancer risk, and misconceptions such as believing darker skin cannot develop skin cancer. Cosmetic dissatisfaction with sunscreen formulations and higher sunscreen prices in lower-income communities were also identified barriers.
Conclusions: Significant disparities in skin cancer outcomes and sun protection behaviors persist among lower SES and SOC patients due to intersecting structural, educational, and healthcare access barriers. Addressing these inequities will require improved patient counseling, culturally inclusive education, better representation in research and training materials, enhanced care coordination, and reduction of financial and access barriers to dermatologic care and sun protection resources. Insights gained through this review and clinical experiences in underserved settings can inform future advocacy and equitable dermatologic practice.