Abstract
Background: Mobile health clinics improve access to care for underserved populations and may reduce emergency department utilization while enhancing chronic disease management. However, these programs face unique challenges in providing longitudinal diabetes care, particularly for uninsured patients experiencing barriers to consistent follow-up. The University of Arizona Mobile Health Program serves uninsured patients throughout southern Arizona while providing interdisciplinary training opportunities for learners.
Objective: To assess glycemic control among family medicine patients with diabetes receiving care through the University of Arizona Mobile Health Program from 2022–2023 and identify opportunities to improve diabetes management despite insurance-related barriers.
Methods: A retrospective chart review was conducted using OneTouch electronic medical record data. Patients were identified using the diagnosis term “diabetes mellitus.” Inclusion criteria included at least one hemoglobin A1C value >6.5%. Patients with prediabetes or gestational diabetes were excluded. Glycemic control was defined according to 2023 American Diabetes Association guidelines: A1C <7.0% for adults aged 18–65 years without major comorbidities and A1C <8.0% for adults aged >65 years or with significant comorbidities. Patients were required to be receiving primary care services and/or be repeat clinic patients. Documentation of foot or eye examinations within the prior year was also assessed.
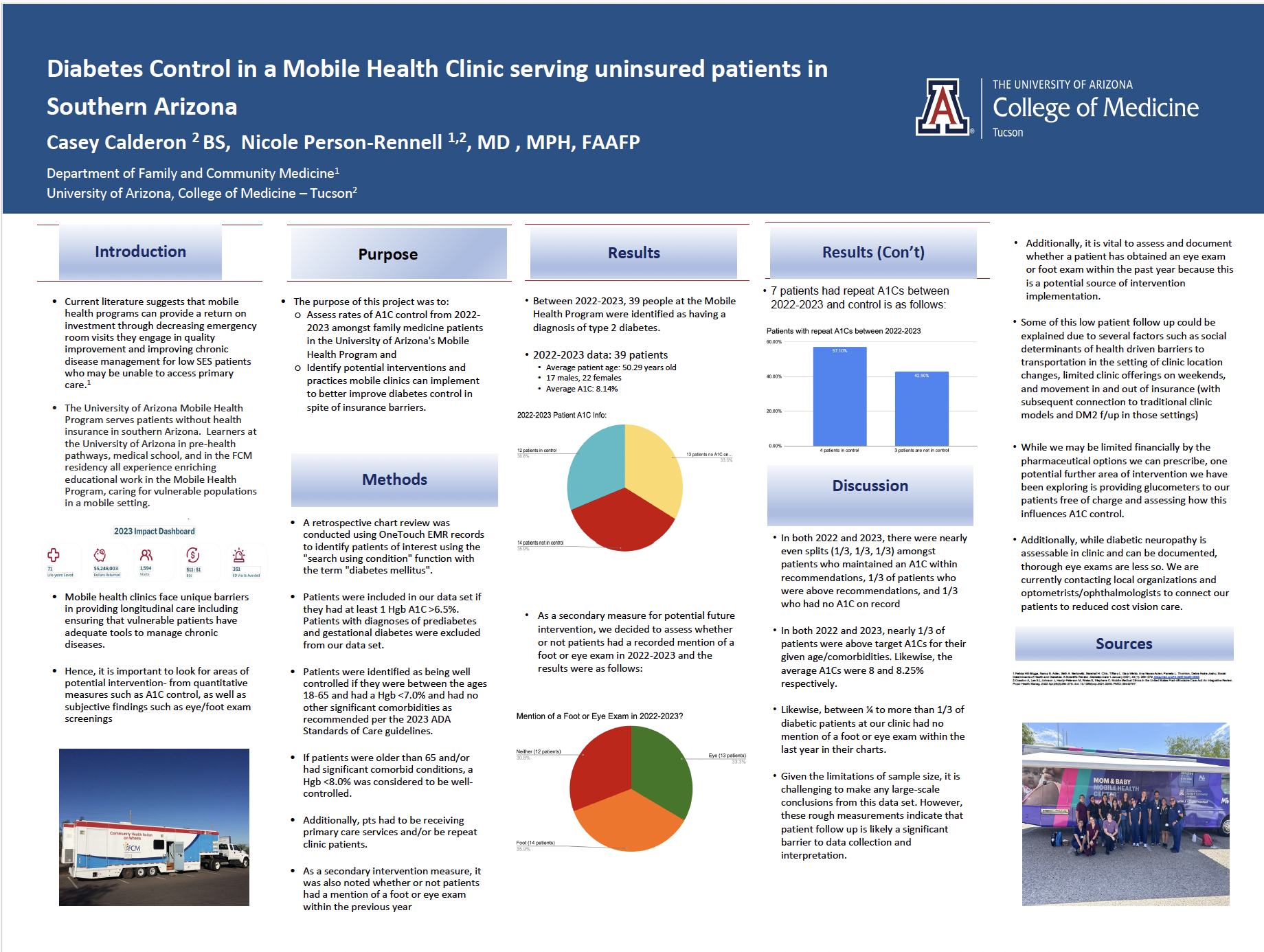
Results: Thirty-nine patients with type 2 diabetes were identified between 2022 and 2023. Mean age was 50.3 years; 17 patients were male and 22 were female. Mean A1C was 8.14%. In both 2022 and 2023, approximately one-third of patients met individualized glycemic targets, one-third remained above target, and one-third had no A1C recorded. Average annual A1C values were approximately 8.0% and 8.25%, respectively. Between one-quarter and more than one-third of patients lacked documentation of a foot or eye examination within the previous year. Seven patients had repeat A1C measurements across both years.
Conclusions: Diabetes management in this uninsured mobile clinic population was limited by inconsistent follow-up and incomplete preventive screening documentation. Social determinants of health, including transportation barriers, changing clinic locations, limited weekend services, and transitions in insurance coverage, likely contributed to these gaps. Potential interventions include provision of free glucometers, enhanced chronic disease outreach, and partnerships to improve access to low-cost ophthalmologic care.