Abstract
BACKGROUND
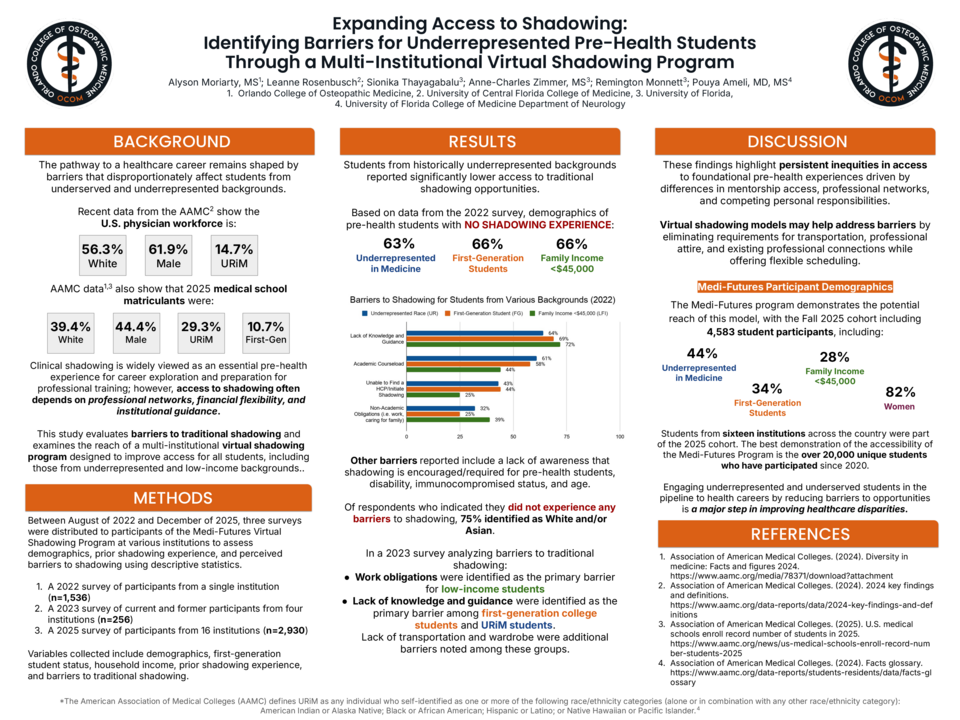
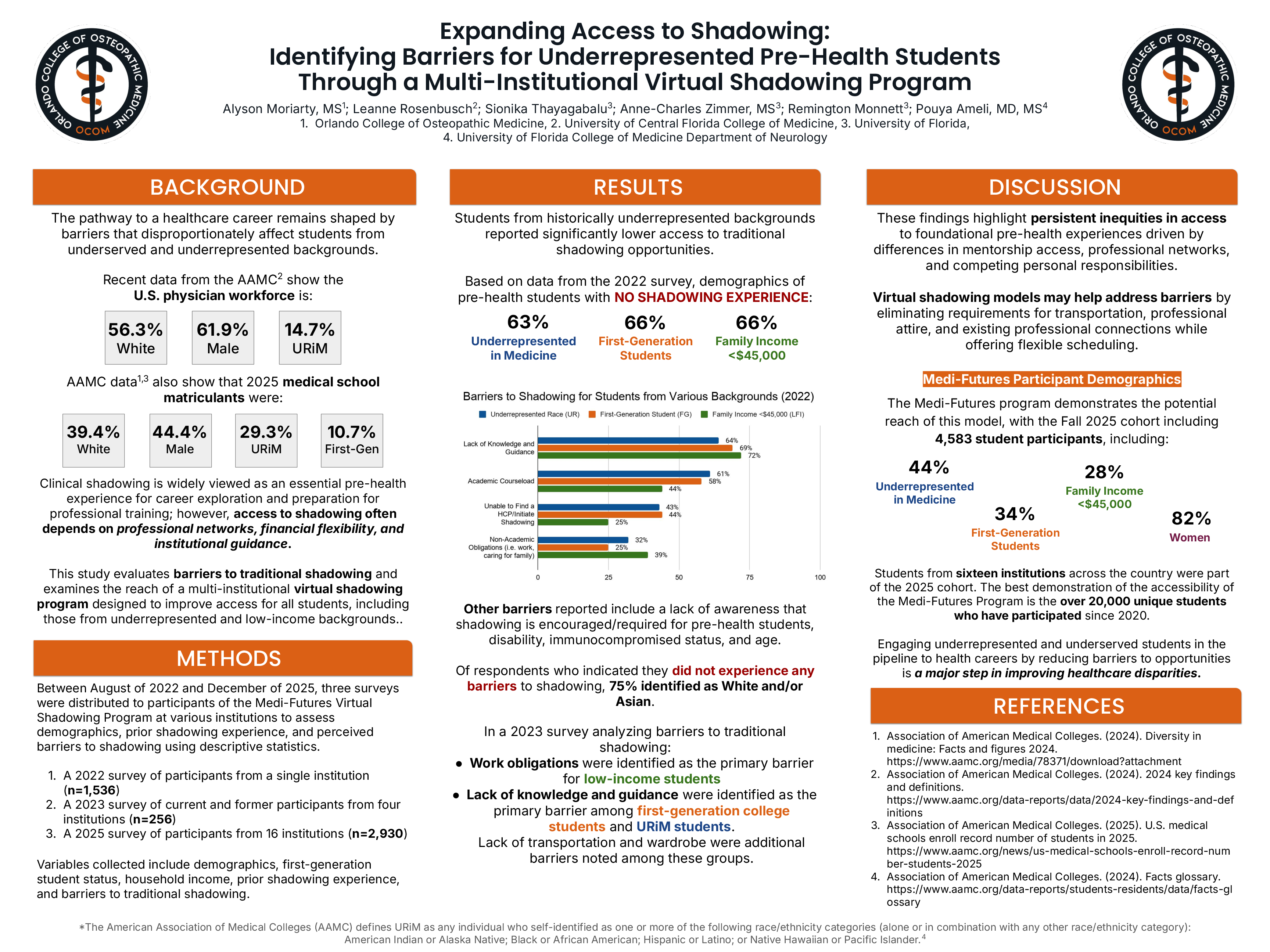
The pathway to a healthcare career remains shaped by barriers that disproportionately affect students from underserved and underrepresented backgrounds. Recent data from the AAMC show the U.S. physician workforce remains predominantly White (56.3%) and male (61.9%), while only 14.7% identify as underrepresented in medicine (URiM) and 10.7% of 2025 medical school matriculants were first-generation college students. Shadowing is widely viewed as an essential pre-health experience for career exploration and professional training preparation; however, access to shadowing often depends on networks, financial flexibility, and institutional guidance. This study evaluates barriers to traditional shadowing and examines the reach of a multi-institutional virtual shadowing program designed to improve access for all students, including those from underrepresented and low-income backgrounds.
METHODS
We analyzed data from three cross-sectional surveys of participants in the Medi-Futures Virtual Shadowing Program: a 2022 survey of participants from a single institution (n=1,536), a 2025 survey of participants from 16 institutions (n=2,930), and a 2023 survey of current and former participants from four institutions (n=256) examining barriers to traditional shadowing. Surveys assessed demographics, prior shadowing experience, and perceived barriers using descriptive statistics.
RESULTS
Across the data, students from underrepresented backgrounds reported substantially lower access to shadowing. In 2022, 63% of URiM respondents, 66% of first-generation students, and 66% of students from households earning <$45,000 reported no prior shadowing experience. Common barriers included lack of professional connections (64% URiM; 69% first-generation), academic workload (61%; 58%), and limited knowledge of how to initiate shadowing (43%; 44%). Among respondents reporting no barriers, 75% identified as White and/or Asian. Similar trends were observed in 2025, where 59% of URiM students, 61% of first-generation students, and 62% of low-income students reported no prior shadowing. Additional analysis in 2023 identified work obligations as the primary barrier for low-income students and lack of guidance for first-generation and URiM respondents.
DISCUSSION
These findings highlight inequities in access to foundational pre-health experiences driven by differences in mentorship access, professional networks, and personal responsibilities. Virtual shadowing models may help address barriers by eliminating the need for transportation, professional attire, and existing connections. The Medi-Futures Program demonstrates the potential reach of this model, with recent cohorts including 44% URiM participants, 34% first-generation college students, and 28% from low-income backgrounds. To improve the diversity within healthcare professions and ultimately contribute to the reduction of health disparities, we should work to improve diversity within the pre-health pipeline.