Abstract
Background: Knee osteoarthritis (KOA) is a degenerative joint disease characterized by
cartilage breakdown and inflammation, representing a leading global cause of disability. Driven by biomechanical wear and pro-inflammatory cytokines, KOA is clinically evaluated via Lawrence KL grading and radiography. Conventional therapies are largely palliative
and frequently culminate in total knee arthroplasty (TKA). To bridge this treatment gap,
intra-articular mesenchymal stem cell (MSC) therapy is increasingly utilized for its chondrogenic and profound immunomodulatory properties. MSCs release a bioactive "secretome" that alters the toxic joint microenvironment to stimulate intrinsic tissue repair. Adipose-derived MSCs (AD-MSCs) and stromal vascular fraction (SVF) are particularly favored in practice for their ease of harvest, high yield, and robust secretory profiles.
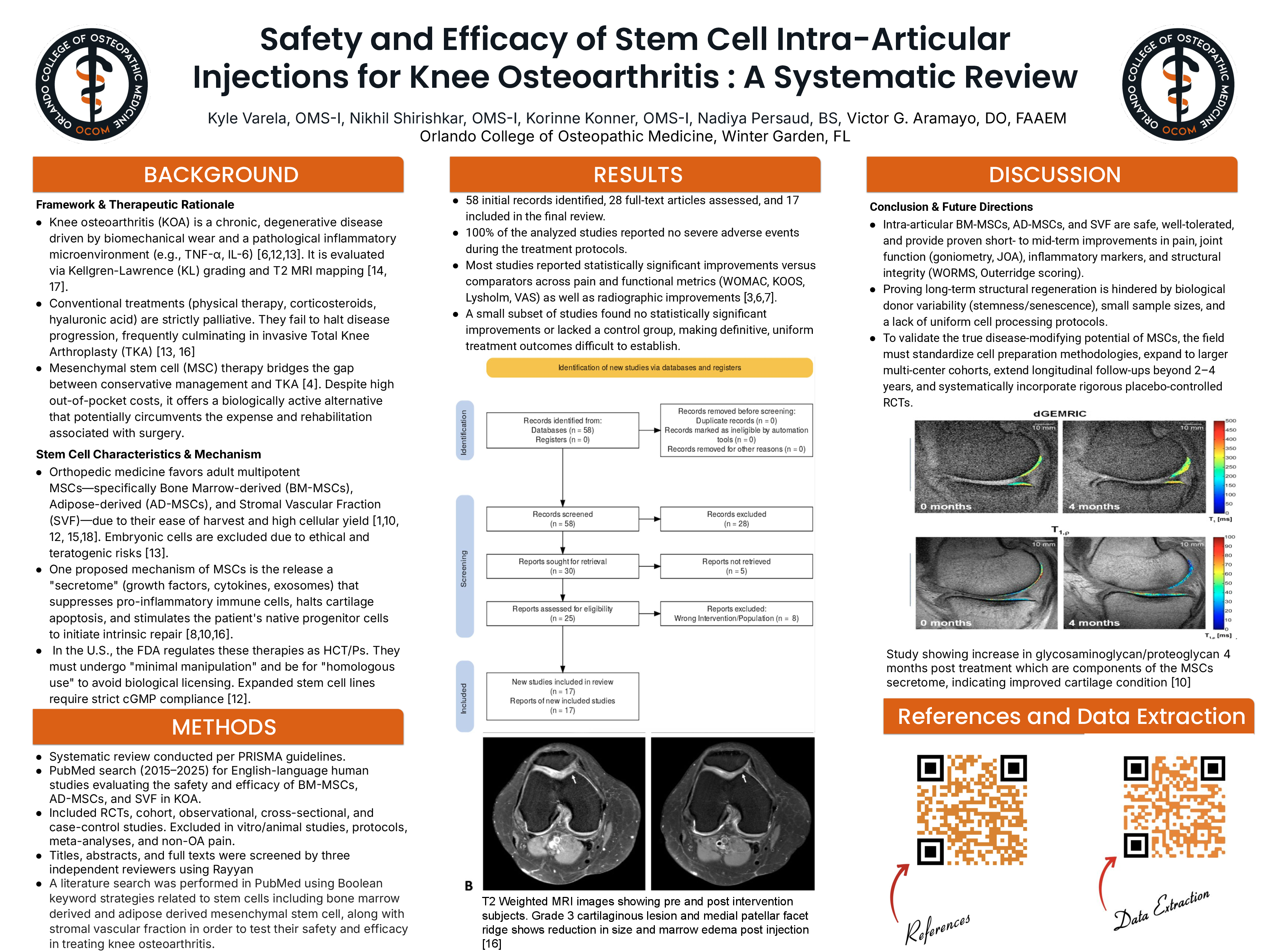
Methods & Results: A total of 58 records were identified across PubMed through PRISMA-guided systematic review (2015-2025). After removal of duplicates and title and
abstract screening, 28 full-text articles were assessed, resulting in 17 studies included in the final review. Included studies primarily consisted of cohort and observational designs, RCTs,
cross-sectional studies, and case control studies examining associations between AD-MSCs, bone-marrow derived MSCs, and SVF injections related to their therapeutic role in KOA including safety and efficacy. Studies including in vitro studies, animal studies, study protocols, meta-analysis, and non-osteoarthritic pain were excluded. Study screening was conducted in Rayyan, where three independent reviewers evaluated titles, abstracts, and full texts based on predefined eligibility criteria. The therapies demonstrated an excellent safety profile, with zero severe adverse events reported across all protocols. The majority of studies showed significant short- to mid-term improvements in clinical outcomes, such as pain reduction, joint function, and radiographic structural integrity compared to control groups or baseline. However, establishing definitive outcomes was occasionally hindered by a lack of proper control groups or statistical significance in a minority of studies.
Discussion: Current evidence strongly supports intra-articular MSC therapy as a safe,
well-tolerated intervention providing short- to mid-term symptomatic and functional relief for
KOA. However, proving definitive long-term cartilage regeneration remains challenging. The
literature is currently limited by donor biological variability, small sample sizes, and inconsistent cell processing protocols. Future research must prioritize standardized methodologies, larger multi-center cohorts, and rigorous placebo-controlled trials with extended follow-ups.