Abstract
Background: Research has found structural differences in mast cell granules between Black and White skin, and that there are increased rates of allergic reactions to food and environmental stimuli in Black populations. Are these findings mostly due to environmental factors or are they mostly associated with genetic predisposition? Prior research has also established the presence of opioid receptors on human mast cells and their propensity to release histamine granules when activated, a pathway that elicits pseudoallergic reactions, most commonly urticaria. When discussing the variations in the IgE mediated histaminergic response, opioid exposure should also be taken into consideration. White patients have been more likely to be prescribed opioids when compared to Black patients, and through these connections, prescribing habits might indirectly hold significance in the incidence of allergic and allergic-type reactions to IV opioids. This paper compares the differences in mast cell reactions to IV opioids in Black and White populations. Previous research surrounding racial differences in opioid binding and cell makeup of the skin creates numerous questions surrounding what physiological differences exist between the mast cells and their activity in Black and White patients.
Objective: The aim of this paper is to compare the incidence of mast cell reactions to IV opioids in Black and White cohorts,with the goal of determining if a significant difference exists between the risk of an allergic reaction when prescribing IV opioids to patients of differing races. This study further examines whether real-life implications result from disparities in prescribing such pharmaceutical agents to Black and White patients.
Methods: This is a retrospective observational study conducted through the TriNetx database. The TriNetX database is a research network composed of electronic medical records (EMRs) of over 100 Health Care Organizations (HCOs). The patient information has been completely deidentified, and the database consists of EMRs from the last 20 years. A White cohort and a Black cohort with identical inclusion and exclusion criteria were propensity score-matched. Given this criteria, a total of 2,520,183 patients were included in this study, 1,262,505 being White patients and 1,257,678 being Black patients. Patients who experienced allergic or allergic-type reactions within 1 day of receiving IV opioids were counted as experiencing an outcome.
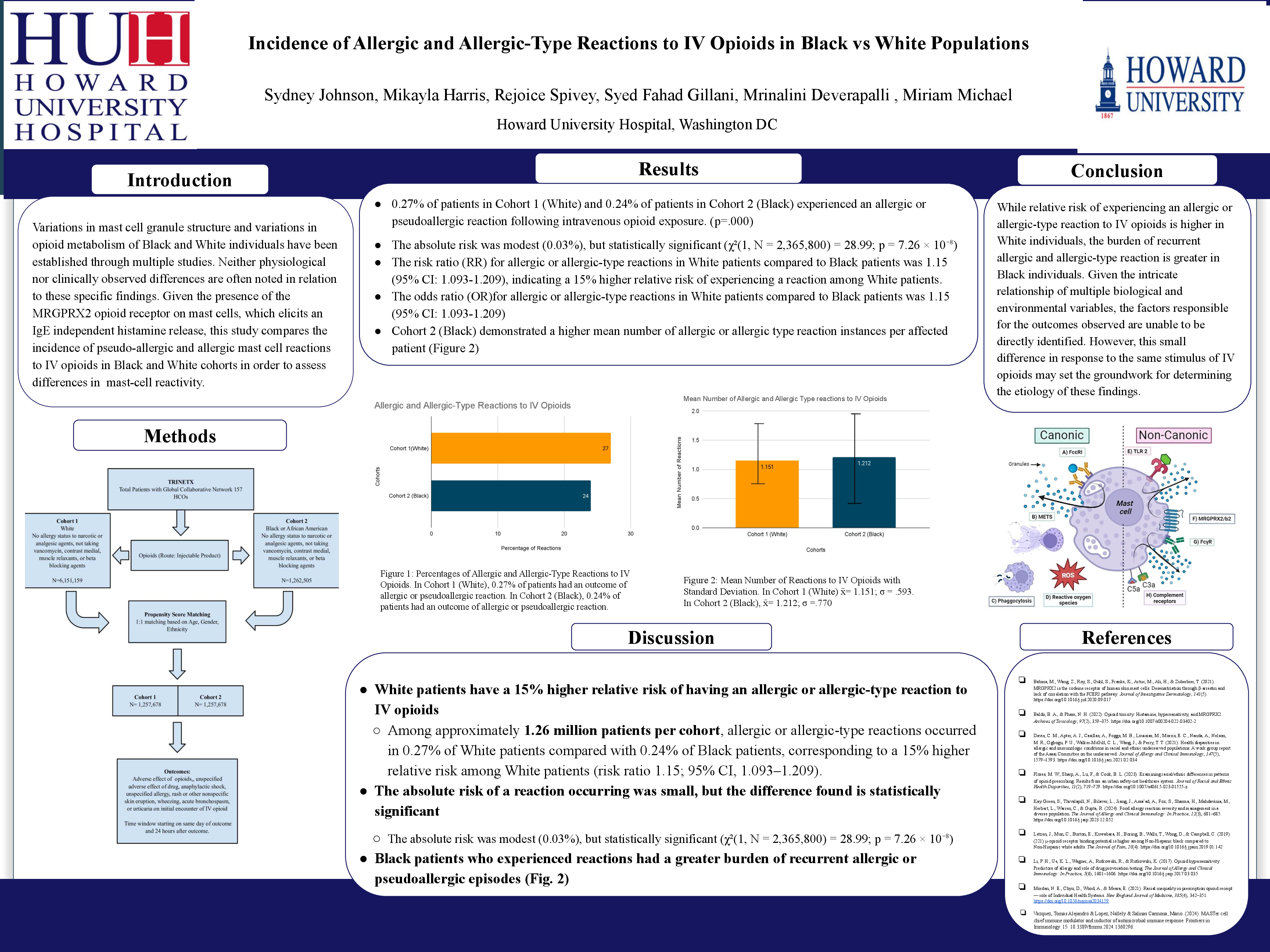
Results: Allergic and allergic-type reactions to opioids are rare (less than 0.3%) in both groups. However, White patients had about a 15% higher chance of being documented as having an allergic-type reaction to opioids in comparison to Black patients. Black patients had a higher rate of repeat reactions. This difference is statistically significant. In a clinical setting, race does not seem to greatly affect the rate of opioid-induced allergic-type reactions.
Conclusion: Statistical difference in the amount of reactions to IV opioids was observed, with White patients having a 15% higher risk of experiencing an allergic or allergic-type reaction to IV opioids than Black patients. Furthermore, these findings provide insight into the possible cellular differences between White and Black patients. The findings of this study could begin to demonstrate differences in mast cell physiology and opioid receptor sensitivity that may or may not be attributed to previously established anatomical variations.