Abstract
BACKGROUND:
When adult patients lack decision making capacity, the principle of “substituted judgement” is typically used to assist in making medical decisions. However, for adult patients who have never had decision making capacity – such as some patients with severe cognitive delay – “best interest” rather than substituted judgement standards must be used. However, ethical challenges can arise when surrogates disagree with clinical recommendations.
CASE:
A 32-year-old woman is admitted to the ICU with severe hyponatremia, Vitamin D toxicity, anemia, and aspiration pneumonia. She weighs 20 kg due to a genetic syndrome, is non-verbal, and has significant cognitive delay. Her parents – who are her primary caregivers and her court appointed legal guardians – routinely give her more than a dozen over the counter vitamins and supplements. These directly contributed to her clinical presentation. Her parents decline recommended blood transfusion and antibiotics as they do not want her to receive blood products with COVID-19 antibodies and because she previously recovered from pneumonia without antibiotics. Clinical Ethics was consulted for guidance.
ETHICAL ANALYSIS/INTERVENTION:
Consideration was given to the role of med-peds trained physicians in providing care for this patient, benefits and harms of interventions, how benefits and harms are defined differently by the medical team and surrogate decision makers, application of the “harm principle”, possibility for iatrogenic harm contributing to the clinical presentation, the impact of state guardianship statues on parental decision-making authority, role of the state given guardianship status, involvement of adult protective services, and opportunities to partner with parents in achieving best interest of the patient.
DISCUSSION/TEACHING POINTS:
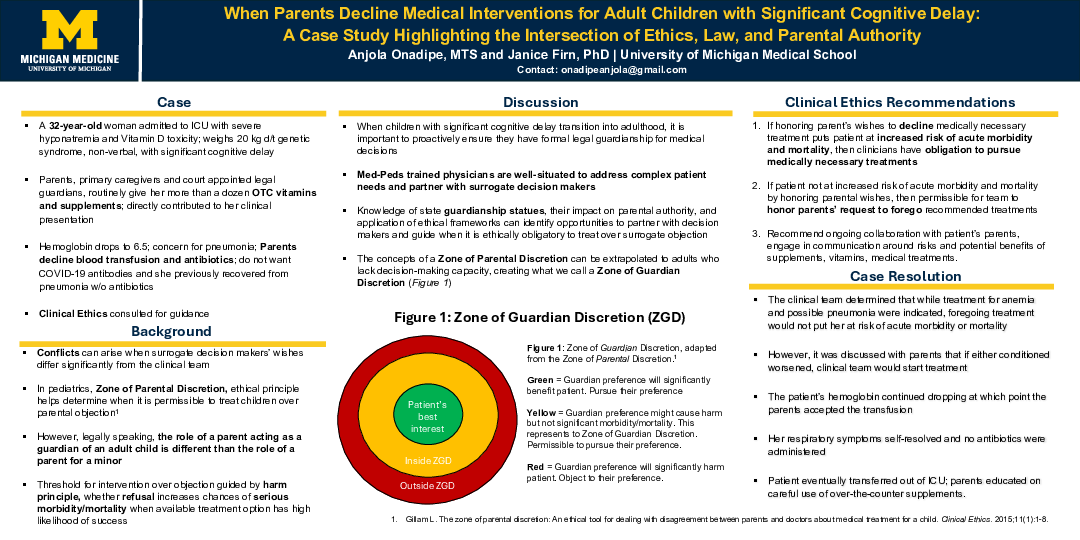
Med-peds trained physicians are well-situated to address complex patient needs and partner with surrogate decision makers. Knowledge of state guardianship statues, their impact on parental authority, and application of ethical frameworks can identify opportunities to partner with decision makers and guide when it is ethically obligatory to treat over surrogate objection.