Abstract
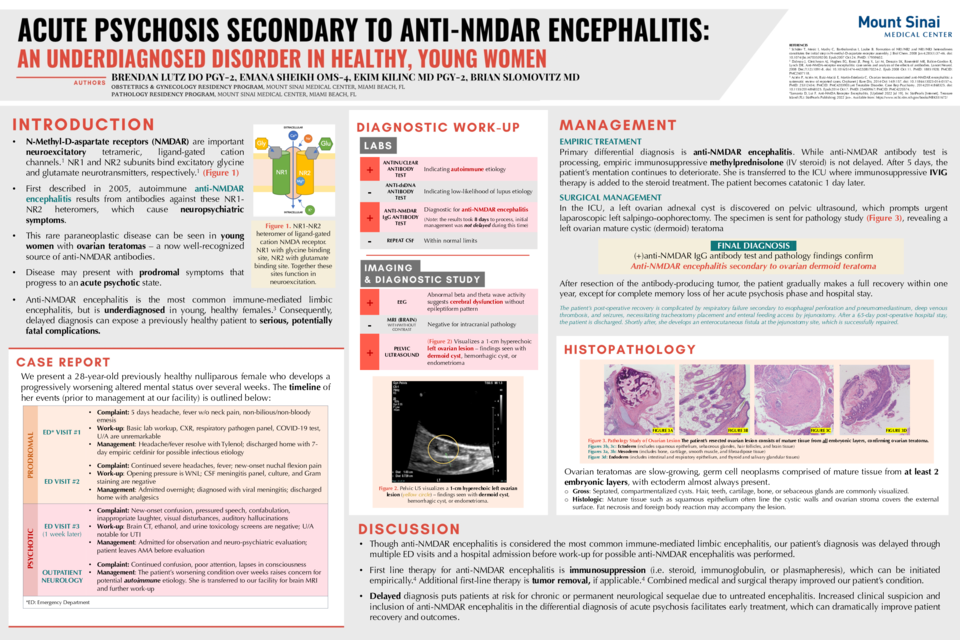
INTRODUCTION: N-Methyl-D-aspartate receptors (NMDAR) are tetrameric, ligand-gated cation channels that play important roles in neuroexcitation. Its NR1 and NR2 subunits form heteromers that bind excitatory glycine and glutamate neurotransmitters, respectively. In 2005, anti-NMDA-receptor encephalitis was first described in which antibodies against these NR1-NR2 heteromers resulted in neuropsychiatric symptoms as a rare, paraneoplastic disease in young women with ovarian teratomas – a now well-recognized source of anti-NMDAR antibodies. Symptoms typically include a vague prodromal state followed by acute psychotic symptoms. Though anti-NMDA encephalitis is considered the most common immune-mediated limbic encephalitis, it is underdiagnosed in young, healthy females. Consequently, delayed diagnosis can expose a previously healthy patient to serious and potentially fatal complications.
CASE DISCUSSION: We describe a healthy 28-year-old nulliparous patient who develops progressively worsening altered mental status, characterized by dysphonia, confabulation, inappropriate laughter, and aggression. After three emergency department visitations, she is assessed by an outpatient neurologist who suspects her erratic behavior refractory to treatment for infectious meningitis to be of autoimmune etiology. The patient is urgently transferred for hospital admission but, the patient’s mentation continues to deteriorate despite empiric anti-NMDAR encephalitis immunomodulatory treatment. Pelvic ultrasound visualizes a left adnexal cyst, prompting urgent laparoscopic left salpingo-oophorectomy, which confirms ovarian teratoma. A positive anti-NMDAR IgG antibody test is diagnostic for anti-NMDAR encephalitis. Though her post-operative recovery is complicated by respiratory failure secondary to esophageal perforation and pneumomediastinum, deep venous thrombosis, seizures, and enterocutaneous fistula, the patient’s status improves and experiences complete recovery within one year, except for complete memory loss of her acute psychosis phase and hospital stay.
DISCUSSION: We present an interesting case of a previously healthy 28-year-old female who demonstrated several weeks of clinically deteriorating mentation. She was seen in the emergency department three times before her mental fluctuations refractory to initial management rose suspicion for possible anti-NMDAR encephalitis. Pelvic ultrasound discovering a left adnexal cyst prompts urgent laparoscopic left salpingo-oophorectomy, further cluing towards anti-NMDAR encephalitis secondary to ovarian teratoma. The patient’s positive anti-NMDAR IgG antibody test is diagnostic for anti-NMDA receptor encephalitis. Though the patient’s post-operative recovery is complicated, combined first-line immunosuppressive treatment and immediate removal of the teratoma markedly improves the patient’s status over a year’s course. In summary, this rare but, well-documented disease, typically seen in women of reproductive age, is frequently caused by anti-NMDAR antibodies produced by ovarian teratomas. Delayed diagnosis puts patients at risk for chronic or permanent neurological sequelae. Increased clinical suspicion of anti-NMDAR encephalitis facilitates early treatment, which can dramatically improve patient recovery and outcomes.