Abstract
Background: Attention Deficient Hyperactivity Disorder or ADHD is a neurological and developmental disorder that manifests in early childhood. Pediatric patients diagnosed with ADHD can be characterized by hyperactive, impulsivity and/or inattention symptoms and can experience marked social, behavioral, and cognitive impairments. Since, ADHD has a complex etiology of environmental, social, and genetic influences, identifying the risk factors are important to tackle this impairing and prevalent condition. Significant adverse childhood experiences from parent(s), parental income and insurance status are some of the ways to conceptualize and measure socio-economic status, which have been explored in this study.
Objective: To understand the association of adverse family events, parental income level, and insurance status on the prevalence of ADD/ADHD in the USA.
Methods: This study is a retrospective cross-sectional study analyzing the 2018-2019 data from National Survey of Children’s health representing U.S. children’s emotional and physical status reported by parents. Adverse childhood experiences (ACE), parental income and insurance status were selected to examine their association with ADHD prevalence among 3–17-year-olds. The primary outcome was currently having, had, or not having an ADD/ADHD diagnosis. A child was considered to have ACE exposure if parents said yes to: divorce or separation, death, and/or incarceration of a parent or a guardian; witnessing violence at home, cohabitation with mentally ill, suicidal, or severely depressed, or with alcohol or drug abusers. ACE variable was further graded into having none, one, or two or more ACEs. Household income responses are stratified to 4 federal poverty levels (FPL): 0-99% FPL, 100-199% FPL, 200-399% FLP, or ≥400% FPL. Insurance status was categorized as having “adequate” or “inadequate” insurance. Data was analyzed and graphed using Python software and MS Excel. The differences between sample counts among the groups were carried out and compared using Chi-square test for independence and odds ratio. All statistical tests were considered significant at a level of 0.05 or less.
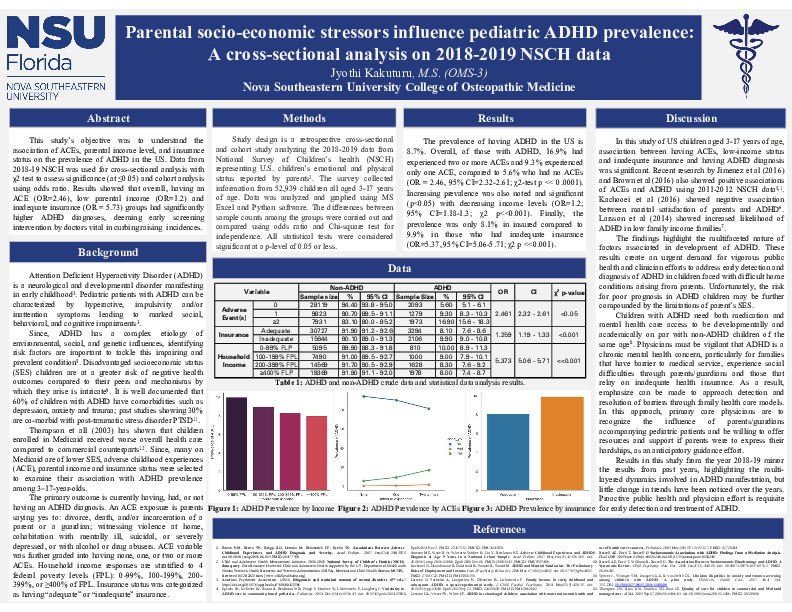
Results: Our final sample included 52939 children. The prevalence of currently having ADHD is 8.7%. Overall of those with ADHD 16.9% had experienced two or more ACEs and 9.3% experienced only one ACE, compared to 5.6% who had no ACEs (OR = 2.46, 95% CI=2.32-2.61; ꭓ2-test p << 0.0001). Increasing prevalence was also noted and significant (p<0.05) with decreasing income levels (OR=1.2; 95% CI=1.18-1.3; ꭓ2 p<<0.001). Finally, the prevalence of ADHD was only 8.1% in insured compared to 9.9% in those who had inadequate insurance (OR=5.37, 95% CI=5.06-5.71; ꭓ2 p <<0.0001).
Conclusions: The study tested the hypothesis that associations would exist between parental behaviors, insurance status, household income levels and ADHD prevalence. Through statistical analysis, parental self-reports of above exposures were positively correlated with parental reports of ADHD in their children. This demands vigorous public health and clinician efforts to address early detection and diagnosis of ADHD in children faced with difficult home conditions arising from parents.