Abstract
Background: Due to the SARS-CoV-2 pandemic, students have been required to navigate new methods of learning, especially since institutions have urgently recreated academic health systems by transitioning to fully online or hybrid platforms. In March 2020, Nova Southeastern University’s College of Osteopathic Medicine transitioned to a fully online platform for preclinical courses, broadcasting live via Zoom and posting recorded lectures online. In September 2020, NSUCOM allowed students the option to attend in person lectures, while also maintaining the online options. It is unclear if and how these curricular changes impact medical students’ emotional and psychological wellness.
Objective: The purpose of this study was to determine which personal factors (Life Stressors, Stress Reduction efforts) or choice of Lecture Modality (asynchronous, online synchronous, and in-person synchronous) significantly contributed to self-reported stress in preclinical first and second year osteopathic medical students.
Methods: An online, anonymous survey was sent to first and second-year medical students in Nova Southeastern University’s College of Osteopathic Medicine in Jan-Feb 2021. Participants were asked to identify the lecture modality they used the most, type of social support, number of stress reduction activities they engaged in, and the presence of life stressors. They self-reported their stress on a novel Likert scale, called the Feeling Stress Scale (FSS). An independent samples t-test was performed on the sample (N=112) to investigate differences in self-reported stress between M1s and M2s. A hierarchical multiple linear regression was calculated to see if the lecture modality, social support, stress reduction activities, or specific life stressors significantly contributed to self-reported stress. Statistical analyses were conducted using SPSS v.26.
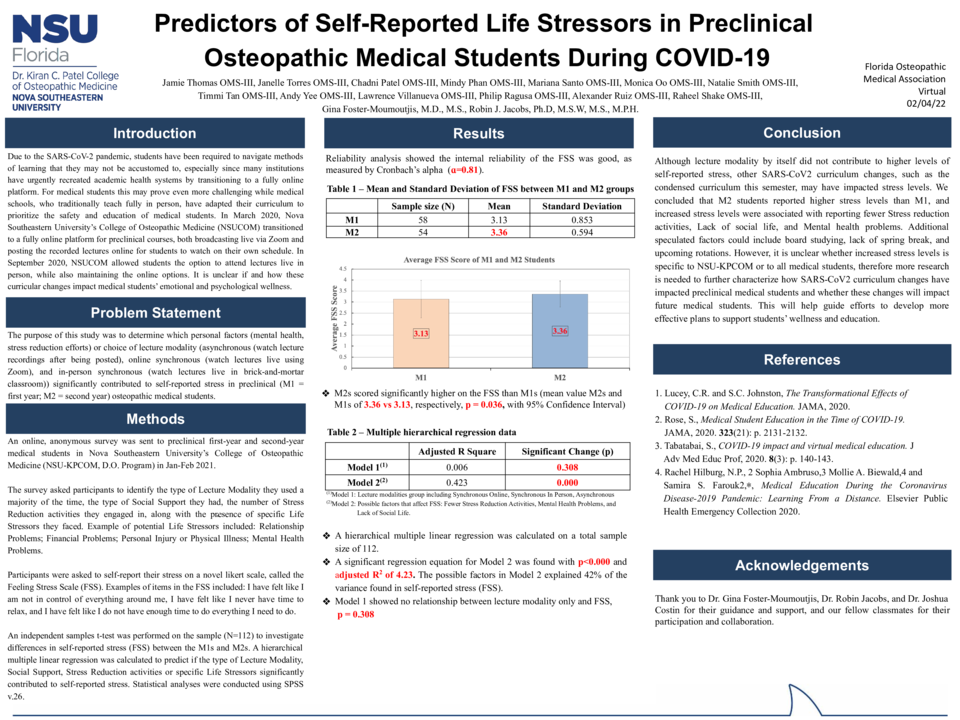
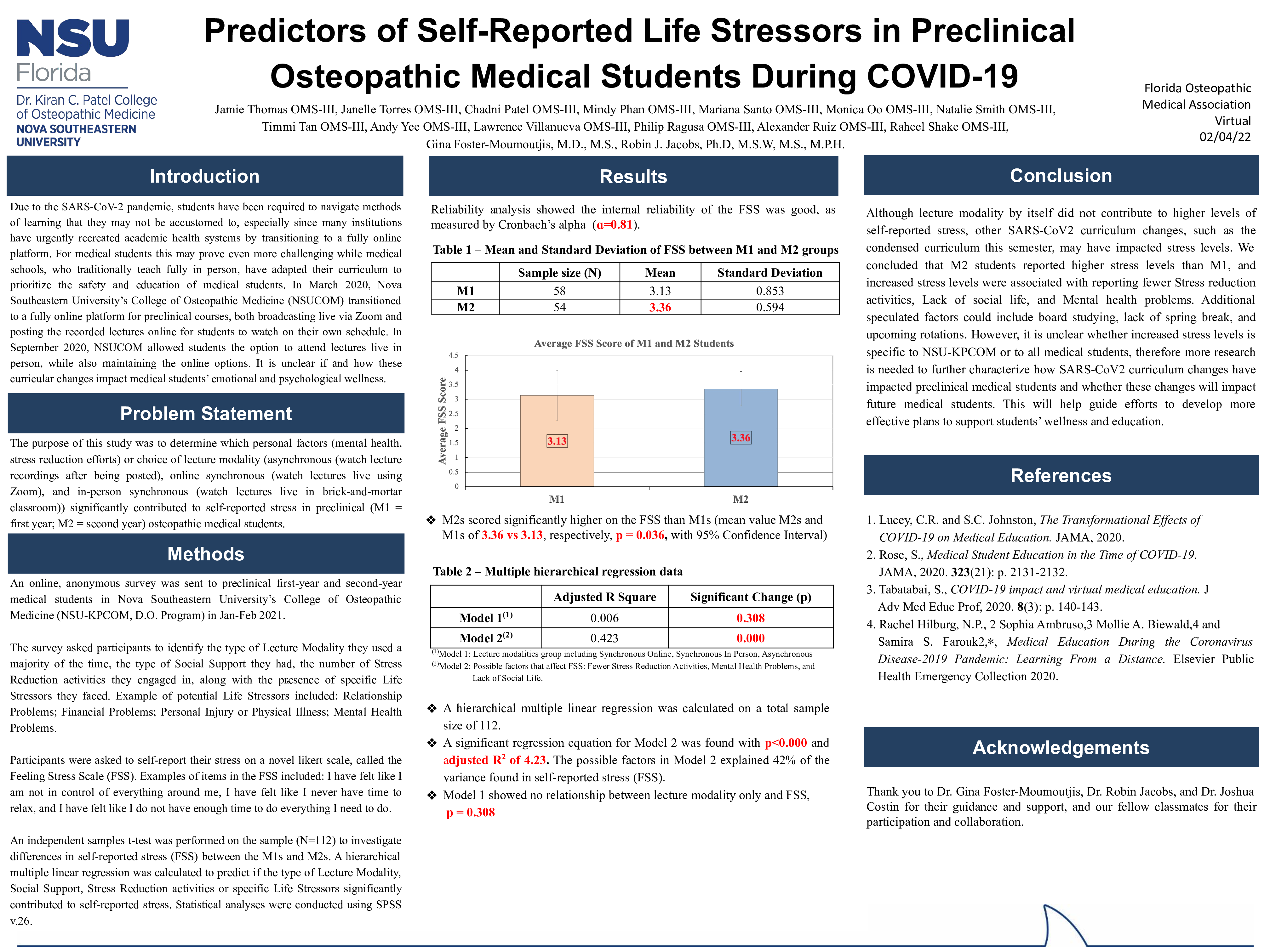
Results: Responses with complete data included 112 pre-clinical medical students, 58 M1 and 54 M2. Mean score on the life stressors scale for the sample was 3.24 (SD=.75, range 1-5). M2s scored significantly higher on the self-reported life stressors scale than M1s (3.36 vs. 3.13; p < .05). Reporting mental health problems, lack of social life, and less engagement in stress reduction activities significantly predicted higher scores on the self-reported stress scale (F(3,108) = 1.215, p <.000), with an R2 of 0.454 (adjusted R2 =0.423); the predictor variables explained 42% of the variance in self-reported stress. Lecture modality (online synchronous vs. asynchronous) did not contribute to self-reported stress.
Conclusion: Although lecture modality by itself did not contribute to higher levels of self-reported stress, other SARS-CoV2 curriculum changes, such as a condensed curriculum, may have impacted stress levels. M2 students reported higher stress levels than M1s. Increased stress levels were associated with fewer reported stress reduction activities, lack of social life, and mental health problems. However, more research is needed to characterize how SARS-CoV2 curriculum changes have impacted preclinical medical students and whether these changes will impact future medical students.