Abstract
Intro:
Healthcare worker (HCW) transmission of Severe Acute Respiratory Syndrome Virus-2 (SARS-CoV-2) that causes COVID-19 disease was a major issue in the early part of the COVID-19 pandemic. It was unclear how effective personal protective equipment (PPE) was in the prevention of this disease. Further, the lack of available PPE made this issue even more difficult to assess. As the understanding of how COVID-19 transmission has increased, it appears that PPE is extremely protective against HCW transmission. This study examines the varying levels of PPE training of physicians and residents, and the specific types of PPE utilized.
Methods:
This study utilized an anonymous survey to assess PPE training and usage in physicians. Physicians and residents from several Southeast Florida teaching hospitals participated in this study. All participants were emailed a link to a standardized questionnaire for demographics information, medical history, current symptoms, PPE use and reuse practices, and PPE training history. An encrypted online survey instrument, Qualtrics, was used to administer the questionnaire from August 2020 to November 2020. The study was approved by the Institutional Review Board of the Florida Atlantic University Schmidt College of Medicine.
Results:
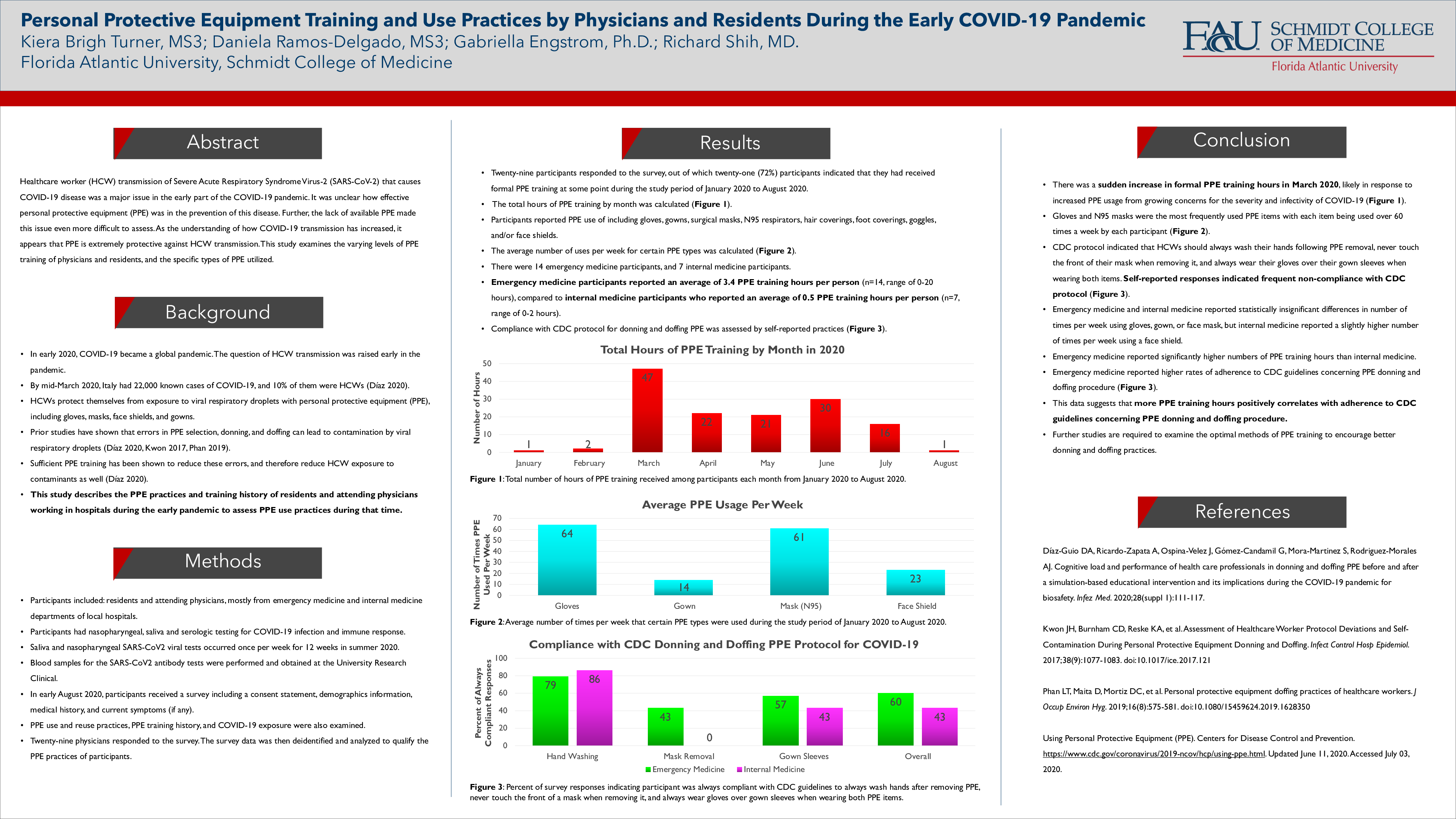
Twenty-nine participants responded to the survey, including fourteen in emergency medicine, eight in internal medicine, and seven in other fields. One of the internal medicine participants did not answer the survey questions regarding PPE practices, and was excluded from analysis. Twenty (71%) participants indicated that they had received formal PPE training at some point during the study period. Their total hours of formal PPE training was 139.5 hours, (mean 7.0 hours, range of 1-75 hours). Twenty-eight participants self-reported adherence to CDC donning and doffing practices by expressing how often they wash their hands following PPE removal, touch the front of their masks when removing, double glove, or wear gloves over their gown sleeves. The fourteen participants from emergency medicine self-reported stricter adherence to the CDC guidelines than the seven included from internal medicine. Emergency medicine participants also reported an average of 3.4 PPE training hours per person (n=14, range of 0-20 hours), compared to internal medicine participants who reported an average of 0.5 PPE training hours per person (n=7, range of 0-2 hours).
Conclusions:
Almost three quarters of physicians received some in-person interactive PPE training during this time. However, many still report frequent mistakes in the donning and doffing of PPE. Further studies should be done to examine the best practices for PPE training.