Abstract
Introduction: There is a growing focus on the growth and retention of a sustainable healthcare workforce in low- and middle-income countries (LMICs). While many factors contribute to the growth and retention of healthcare workers, a sustainable workforce requires protection from workplace violence (WPV). Previous studies in the US and LMICs have reported that 60-87.5% of emergency healthcare providers (e.g. nurses and physicians) experience some form of WPV annually. Most providers report frequent verbal assault (VA), and studies suggest a wide range (15-65%) of physical assault (PA) experiences in the workplace. Emergency Medical Technicians (EMTs), an emerging workforce in many LMICs, often work in unregulated, unpredictable, and dynamic environments. As a result, we hypothesized that these prehospital providers experience high rates of WPV. To our knowledge, no previous studies have evaluated violence experienced by EMTs in LMICs.
Methods: This was an exploratory study to establish the prevalence of WPV experienced by EMTs in India. We administered a cross-sectional survey to EMTs presenting for educational sessions at GVK Emergency Management and Research Institute (EMRI) in four Indian States (Gujarat, Karnataka, Tamil Nadu and Telangana). Surveys were completed from July to November 2017. The survey instrument was adapted from the Joint Program on Workplace Violence in the Healthcare Sector (ILO/ICN/WHO/PSI) which has been frequently used in other global settings. The survey was translated and back translated into local languages (Gujarati, Kannada, Tamil and Telugu) to ensure accuracy.
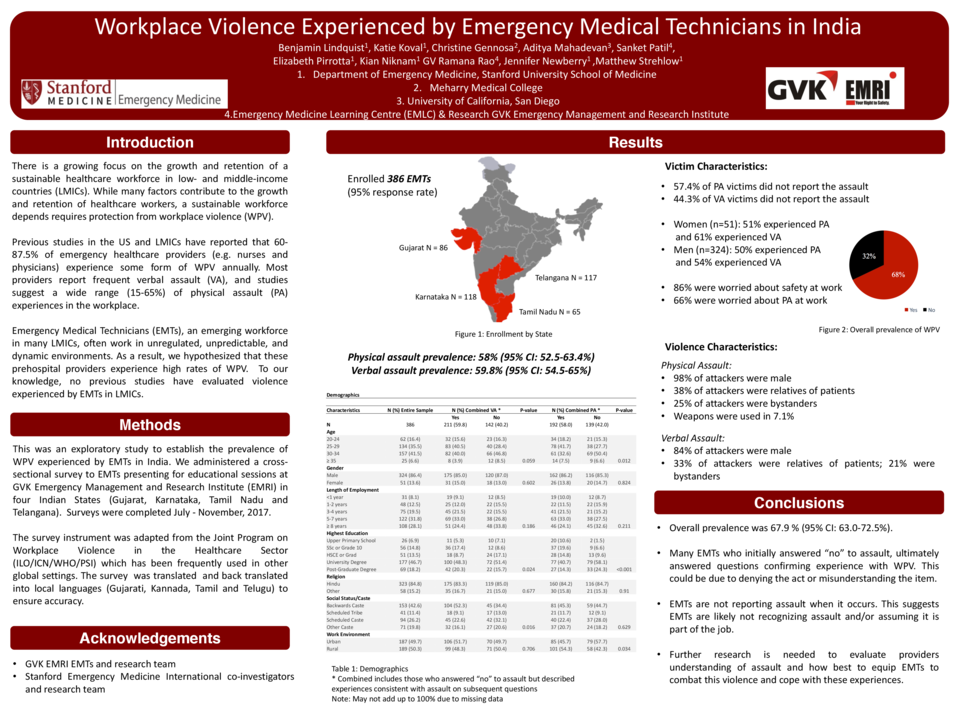
Results: In total, 386 EMTs completed the survey (95% response rate) from Gujarat (86), Karnataka (118), Tamil Nadu (65) and Telangana (117). Most were men (86.4%). Overall prevalence of workplace violence was 67.9% (95% CI; 63.0-72.5%). PA prevalence was 58% (95% CI: 52.5-63.4%) and VA prevalence was 59.8% (95% CI: 54.5-65%). Many victims (57.4% of PA and 44.3% of VA) did not report the assault at the time of the incident. Most attackers were male (98% for PA and 84% for VA) and relatives of the patient (38%). Of the PA cases, 7.1% involved a weapon.
Conclusions: Compared with other studies of LMIC healthcare providers, we found a slightly higher prevalence of physical assault. We found that many EMTs who initially answered “no” to assault, ultimately answered questions confirming experience with WPV. Additionally, EMTs are often not reporting assault when it occurs. Further research is required to evaluate providers understanding of assault and how best to equip EMTs to combat this violence and cope with these experiences.