Abstract
Background: Competency-based medical education (CBME) is playing a central role in today’s training of resident physicians. There is a need to develop adequate training and assessment tools, including simulation, to ultimately deliver competent physicians, capable of unsupervised practice.
Objectives: The aim of this Delphi survey is threefold: first, to quantify the importance of each Entrustable Professional Activity (EPA) with respect to Obstetrics & Gynecology (OBGYN) residency training, second, to set benchmark levels for each EPA, and third, to identify the importance of simulation-based training and assessment for each EPA.
Methods: The individual items (EPAs) used in the survey were defined based on literature review of five OBGYN curricula worldwide. Two rounds of a modified Delphi method via online questionnaire through “Survey Monkey” were performed. Experts in the study were OBGYN residency program directors across Canada and United States. Experts rated the importance of each EPA for residency training, identified benchmark levels of competence for predefined stages of training, and roles of simulation-based training and assessment. A Likert scale was used (1 to 5); consensus was defined as ≥80% agreement.
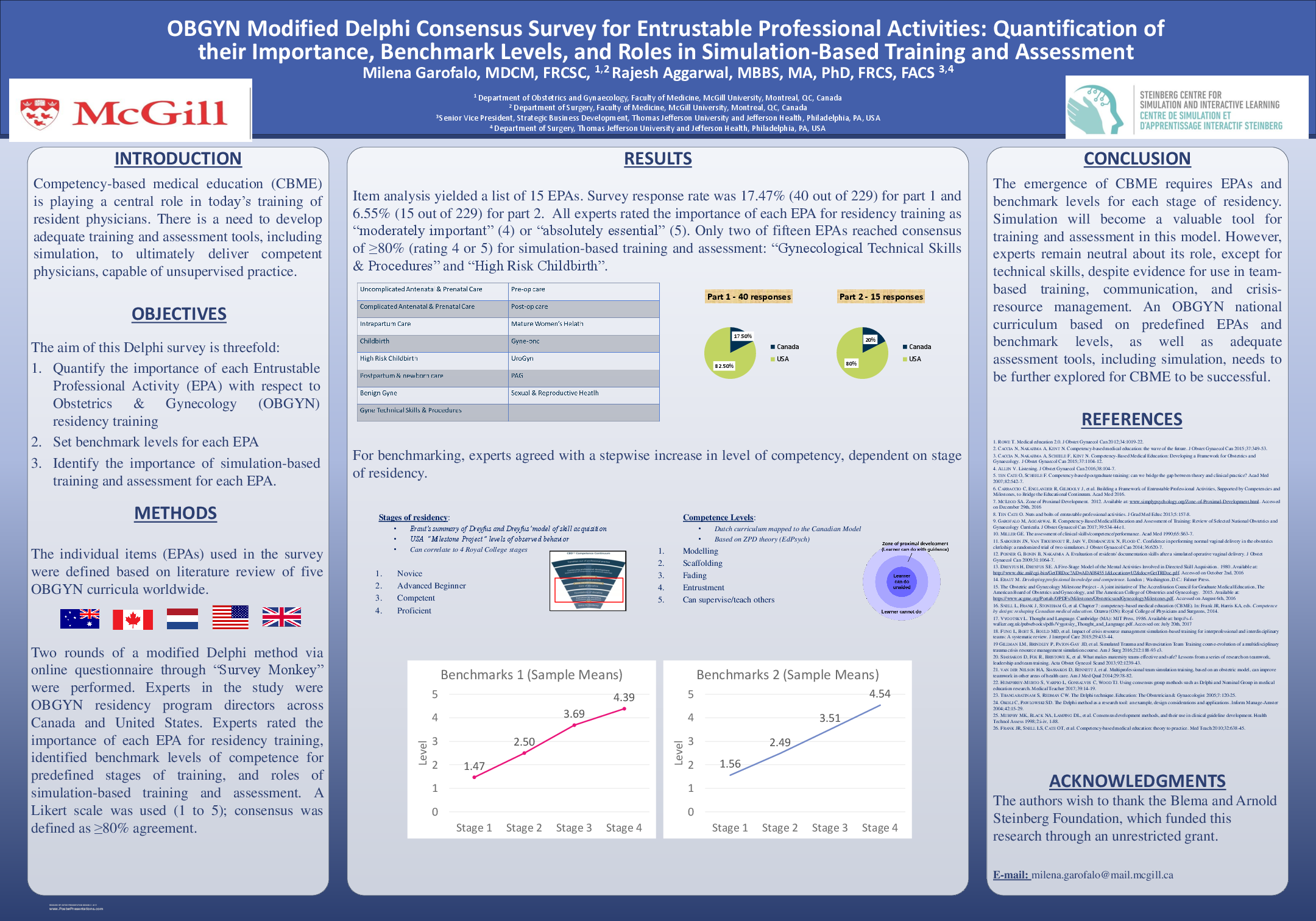
Results: Item analysis yielded a list of 15 EPAs. Survey response rate was 17.47% (40 out of 229) for part 1 and 6.55% (15 out of 229) for part 2. All experts rated the importance of each EPA for residency training as “moderately important” (4) or “absolutely essential” (5), validating the 15 EPAs. For benchmarking, experts agreed with a stepwise increase in level of competency, dependent on stage of residency. Only two of fifteen EPAs reached consensus of ≥80% (rating 4 or 5) for simulation-based training and assessment: “Gynecological Technical Skills & Procedures” and “High Risk Childbirth”.
Conclusion: The emergence of competency-based medical education (CBME) requires EPAs and benchmark levels for each stage of residency. Simulation will become a valuable tool for training and assessment in this model. However, experts remain neutral about its role, except for technical skills, despite evidence for use in team-based training, communication, and crisis-resource management. An OBGYN national curriculum based on predefined EPAs and benchmark levels, as well as adequate assessment tools, including simulation, needs to be further explored for CBME to be successful.